Surgical Site Drains: Benefits and Risks
Why do some patients need a surgical drain?
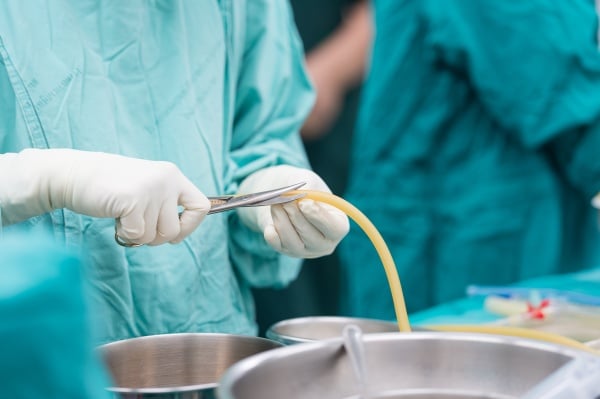
Surgical wound dehiscence and surgical site infections are major postoperative complications that significantly impact patient morbidity, mortality, economic burden, and quality of life. A factor in surgical wound dehiscence and infection is postoperative dead space and fluid accumulation. Dead space is an area that develops between tissues after disruption of subcutaneous connective tissues. It is undesirable because the fluid that typically fills this void provides a prime medium for bacterial growth. Fluid accumulation can also cause internal pressure to the surgical site — as well as adjacent organs, nerves, and blood vessels — and impact tissue perfusion and wound healing.
What types of surgical drains or drainage systems are available?
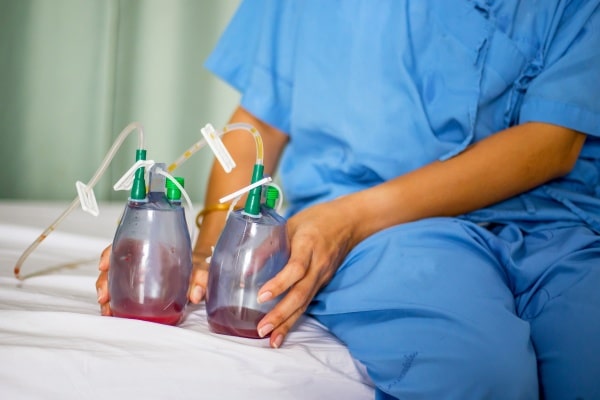
Various types of wound drains or drainage systems are used to prevent the aforementioned issues from occurring. A drain inserted at the time of surgery provides a route through which air and body fluids can be evacuated from the operative site. They are classified as: open or closed, and passive or active. Passive drains rely on gravity, body movement, pressure differentials, or overflow to move fluid or gas. Active drains use intermittent or continuous negative pressure to pull fluid or gas from a wound or body cavity. The type of drainage system inserted is based on the needs of the patient, type of surgery, type of wound, amount of drainage expected, and surgeon preference.
What are some surgeries that commonly use drains?
Examples of surgeries that commonly use drains or drainage systems include:
-
Biliary surgery
-
Breast surgery
-
Chest surgery
-
Contaminated surgical cases
-
Infected cysts surgery
-
Orthopedic surgery
-
Pancreatic surgery
-
Plastic surgery
-
Neurosurgery
-
Thyroid surgery
What complications can arise from surgical drains?
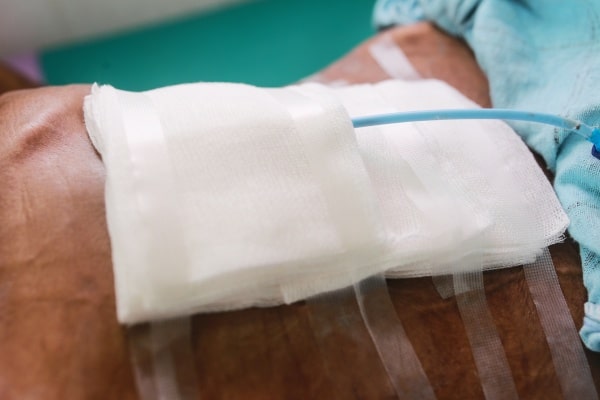
Drains are not without complications. Despite meticulous placement, instructions for care, and timely removal by the surgeon, complications may still occur. These include tissue inflammatory reactions or insertion site necrosis from the pressure of the drain tubing to the surrounding intact skin. The drain may also be a source of contamination if it becomes clotted, becomes clogged, or becomes a conduit allowing opposite flow within it, thus increasing the possibility of surgical site infection.
What evidence supports the use of surgical drains?
While surgical drains are still commonly used and the complication rates are low, there is a lack of definitive evidence in the literature regarding their application. Solutions to eliminate drains whenever possible are trending. Negative Pressure Wound Therapy use over closed surgical incisions has been shown to be beneficial in reducing rates of surgical site infection, seroma/hematoma, and dehiscence, and improving scar quality as an alternative. The use of hydrolyzed collagen powder is another alternative/adjunctive form of dead space management reported.
To learn more about a product that manages surgical wounds, please visit https://sanaramedtech.com/surgical/celleraterx-surgical/
References:
– Durai R, Mownah A, Ng PC. Use of drains in surgery: a review. J Perioper Pract. 2009 Jun;19(6):180-6.
– Hyldig N, Birke-Sorensen H, Kruse M, et al. Meta-analysis of negative-pressure wound therapy for closed surgical incisions. Br J Surg 2016; 103; 477-86.
– Russel J, Koltz PR. Dead Space Management in Plastic Surgery: A Systematic Review of Current Techniques and Products. American College of Plastic Surgery Conference 2020 abstract presentation.




