Caring For Your Feet After A Surgical Nail Removal
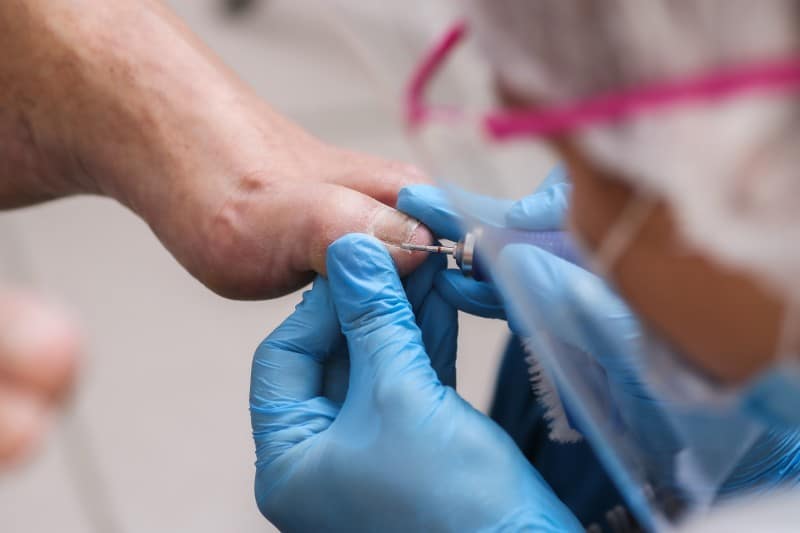
What Happens After Your Toenail or Fingernail Is Removed?
The loss of a toenail or fingernail may be the result of trauma or due to a planned removal as a course of treatment for an ingrown nail, infection, or for evaluation of the tissue below the nail. Surgical nail removal is usually performed when a large portion of the nail is diseased and damaged or if your nails are very painful. Care of the nail removal site focuses on an appropriate environment for healing, prevention of excessive bioburden that may cause infection, and pain management. It may take up to 6 months for a fingernail or about 6 to 12 months for a toenail to fully grow back.
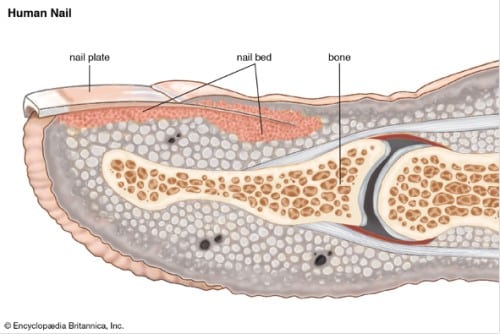
How Can You Protect Your Nail Bed?
The nail bed is moist, soft and very sensitive. The area will need to be protected and kept in an environment conducive to healing. An antimicrobial skin and wound cleanser followed by an antimicrobial hydrogel wound dressing can address microbes that can contaminate the site while providing a moist wound healing environment. A nonadherent, absorbent secondary dressing may then be applied as bandages tend to stick to a newly exposed nail bed. The dressing is typically changed every 1-2 days, including cleansing with an antimicrobial skin and wound cleanser unless directed otherwise.
Follow your healthcare provider’s directions as advised. They will usually involve elevation as much as possible for the first 48 hours to keep swelling at a minimum to the affected digit. Take pain medication as your provider has prescribed or recommended. Antibiotics may have been prescribed for an infection and should be taken as directed.
When Should You Contact Your Healthcare Provider?
Be sure to contact your healthcare provider if you experience:
- increasing pain and swelling after 24 hours
- redness around the nail or digit, or fluid draining from your finger or toe
- any red streaking developing
- development of a fever 100.4 degrees or higher, or otherwise as directed by your provider
To learn more about Sanara MedTech products, please visit. https://sanaramedtech.com/surgical/